Sleep Latency Explained: The 15-Minute Sweet Spot
Most people think falling asleep fast is a sign of good sleep. It isn't always. The time it takes you to fall asleep — your sleep latency — is one of the most useful and most misunderstood numbers your tracker shows you.
Key Insight: Healthy adults fall asleep in 10 to 20 minutes. Under 8 minutes can signal sleep debt. Over 30 minutes can signal insomnia. The number tells you something different depending on which side of normal you're on.
What Is Sleep Latency?
Sleep latency, also called sleep onset latency or SOL, is the time it takes you to fall asleep after lights out. The clock starts the moment you decide to sleep — eyes closed, lights off — and stops the moment you cross into stage N1, the lightest stage of sleep.
Sleep medicine treats SOL as one of four core sleep metrics, alongside total sleep time, wake after sleep onset, and sleep efficiency. Together, these tell a doctor how well your sleep system is working.
Your latency reflects two things: how much sleep pressure has built up across the day, and how relaxed your nervous system is when you get into bed. High pressure plus low arousal equals a fast, smooth sleep onset. Low pressure or high arousal stretches the wait.
Sleep pressure is driven by adenosine, a chemical that builds up the longer you're awake. The more you have, the sleepier you feel. Caffeine works by blocking adenosine receptors, which is exactly why a late-afternoon coffee can stretch your latency by 30 minutes or more. Arousal is the other side — it's the level of activation in your sympathetic nervous system. Stress, screens, alcohol, and a warm room all push it up.
A useful way to think about latency is as a window into the balance between these two systems. When the number drifts in either direction, it's telling you something specific about which one is off.
What's Normal?
The American Academy of Sleep Medicine (AASM) describes a normal sleep latency as somewhere between 10 and 20 minutes. The mean for healthy adults on the standardized clinical test is around 11 minutes.
A latency under 8 minutes on a clinical test is one of the diagnostic markers for excessive daytime sleepiness. A latency over 30 minutes most nights is one of the criteria the DSM-5 uses to define insomnia disorder, alongside daytime impairment and a frequency of at least three nights per week.
The 15-minute sweet spot isn't arbitrary. It reflects a body that's tired enough to sleep but not so exhausted it crashes the moment it stops moving.
The number can also drift around night to night. A latency of 25 minutes after a stressful day, or 8 minutes after a brutal workout, doesn't mean anything is wrong. Look at the average across a full week. That's what gives you signal instead of noise.
Why Falling Asleep Too Fast Is a Warning Sign
"I sleep so well, I'm out as soon as my head hits the pillow." That's actually a red flag. Falling asleep in under 5 minutes is what sleep researchers call pathological sleepiness. It means you've built up so much sleep pressure that your brain is jumping at the first chance to discharge it.
A 2010 review in Industrial Health found that shift workers with shift work disorder have a mean sleep latency of just 4.8 minutes during clinical testing — half the normal value. People with chronic short sleep show similar patterns.
The cost of running a 4-minute latency every night isn't dramatic in any one moment. But over months, the chronically under-slept brain accumulates measurable cognitive and metabolic damage. If you're proud of falling asleep in 2 minutes, see our piece on sleep debt — you may be running a deficit.
Who Tends to Have Very Short SOL
- •Shift workers and people with rotating schedules
- •People sleeping less than 6 hours regularly
- •New parents and caregivers
- •People with untreated sleep apnea or narcolepsy
The MSLT: How Doctors Test Sleep Latency
The clinical gold standard for sleep latency is the Multiple Sleep Latency Test (MSLT). It's run in a sleep lab the day after an overnight sleep study. You're given five 20-minute nap opportunities, two hours apart, in a dark, quiet room.
The technician measures how long it takes you to fall asleep on each nap and averages them. The mean MSLT is the number that drives clinical decisions:
< 5 minutes
Severe sleepiness. With two REM-onset naps, this can confirm narcolepsy.
5–10 minutes
Moderate sleepiness. Suggests significant sleep debt or untreated sleep disorder.
10–15 minutes
Borderline. Worth investigating but not clearly abnormal.
> 15 minutes
Normal alertness. The healthy zone.
You won't get an MSLT unless your doctor orders one, but the same thresholds inform what your wearable is telling you. They're a useful frame for reading your own latency data.
One important difference: the MSLT measures how fast you fall asleep during the day, when you're supposed to be alert. Your at-home sleep latency measures how fast you fall asleep at night, when you're supposed to feel sleepy. The two numbers are related but they're not the same thing. A person with a long nighttime latency can still have a very short daytime MSLT — that's the classic profile of someone with insomnia who's so tired during the day their brain is desperate for any sleep it can get.
How Age Changes Sleep Latency
Sleep latency drifts upward with age. A healthy 25-year-old typically falls asleep in 10 to 15 minutes. By 65, the same person might take 20 to 25. This is partly biology — older adults have weaker circadian signals — and partly accumulated worry, medication effects, and physical discomfort.
Children show the opposite. A well-rested toddler can take 20 to 30 minutes to fall asleep because their sleep pressure builds more slowly. Teenagers, on the other hand, often have biologically delayed circadian rhythms that push their natural sleep onset toward midnight or later.
If you're noticing your latency creeping up year over year, it's not necessarily a problem — but it is worth tracking alongside your overall sleep quality and sleep score.
How Apple Watch and Reverie Estimate SOL
Wearables can't read your brainwaves, so they estimate sleep onset using two main signals: heart rate decline and motion. When you're awake in bed, your heart rate stays elevated and your wrist makes small movements. When you cross into N1, both drop sharply.
Apple Watch Series 4 and later, running watchOS 9 or newer, uses these signals plus blood oxygen and HRV to flag the moment of sleep onset. The estimate is usually within a few minutes of polysomnography, though it tends to underestimate latency in people who lie very still while awake.
Reverie pulls the same Apple Watch data and shows you SOL alongside the habits and conditions that influenced it — caffeine timing, room temperature, exercise, screen use. That's where the number turns from a curiosity into a lever.
A few caveats worth knowing. Wearables tend to misread "lying still and reading" as sleep, which can make your latency look shorter than it really is. They also miss the very brief micro-arousals that happen at sleep onset. The wrist signal is good enough to spot trends across weeks, but don't put too much weight on any single night.
For the most accurate read, start the sleep tracker only when you've actually decided to sleep — lights off, eyes closed. If you scroll your phone in bed for 30 minutes first, your tracker will likely call that wake time anyway, but the boundary will be cleaner if you just close your eyes when you're ready.
How to Adjust Your Sleep Latency
Whether you need to widen or shrink your latency depends on where you sit on the curve.
If Your SOL Is Too Long (> 30 min)
- • Try the techniques in our how to fall asleep faster guide — cognitive shuffle, 4-7-8 breathing, paradoxical intention.
- • Cool the bedroom to 65–68°F.
- • Stop caffeine at least 8 hours before bed.
- • Don't get into bed until you actually feel sleepy.
- • If anxiety drives your wakefulness, see our piece on sleep and anxiety.
If Your SOL Is Too Short (< 5 min)
- • You're almost certainly not sleeping enough. Add 30 to 60 minutes to your nightly sleep window.
- • Move bedtime earlier rather than wake time later — morning light protects circadian timing.
- • If you snore loudly or wake gasping, get screened for sleep apnea.
- • Track your latency for two weeks. If it stays under 5 minutes despite a longer sleep window, talk to a sleep doctor.
See Your SOL Trend in Reverie
Reverie pulls your sleep latency from your Apple Watch and charts it across weeks. You'll see whether your number is creeping up, dropping into the danger zone, or holding in the healthy 10–20 minute range.
- • Track sleep latency night by night
- • Spot which habits move it
- • Compare weekday vs weekend onset
- • Get insights when your trend shifts
References
- Littner MR, et al. "Practice parameters for clinical use of the multiple sleep latency test and the maintenance of wakefulness test." Sleep. 2005;28(1):113-121. AASM
- Krahn LE, et al. "Recommended protocols for the Multiple Sleep Latency Test and Maintenance of Wakefulness Test in adults: guidance from the American Academy of Sleep Medicine." Journal of Clinical Sleep Medicine. 2021;17(12):2489-2498. JCSM
- Wright KP Jr, et al. "Shift work and the assessment and management of shift work disorder (SWD)." Sleep Medicine Reviews. 2013;17(1):41-54. PubMed
- Ohayon MM, et al. "Meta-analysis of quantitative sleep parameters from childhood to old age in healthy individuals." Sleep. 2004;27(7):1255-1273. PubMed
- Walker MP. Why We Sleep: Unlocking the Power of Sleep and Dreams. Scribner. 2017. Sleep Foundation overview
- Drake C, et al. "Shift Work Sleep Disorder: Prevalence and Consequences Beyond That of Symptomatic Day Workers." Sleep. 2004;27(8):1453-1462. PubMed
Related Articles
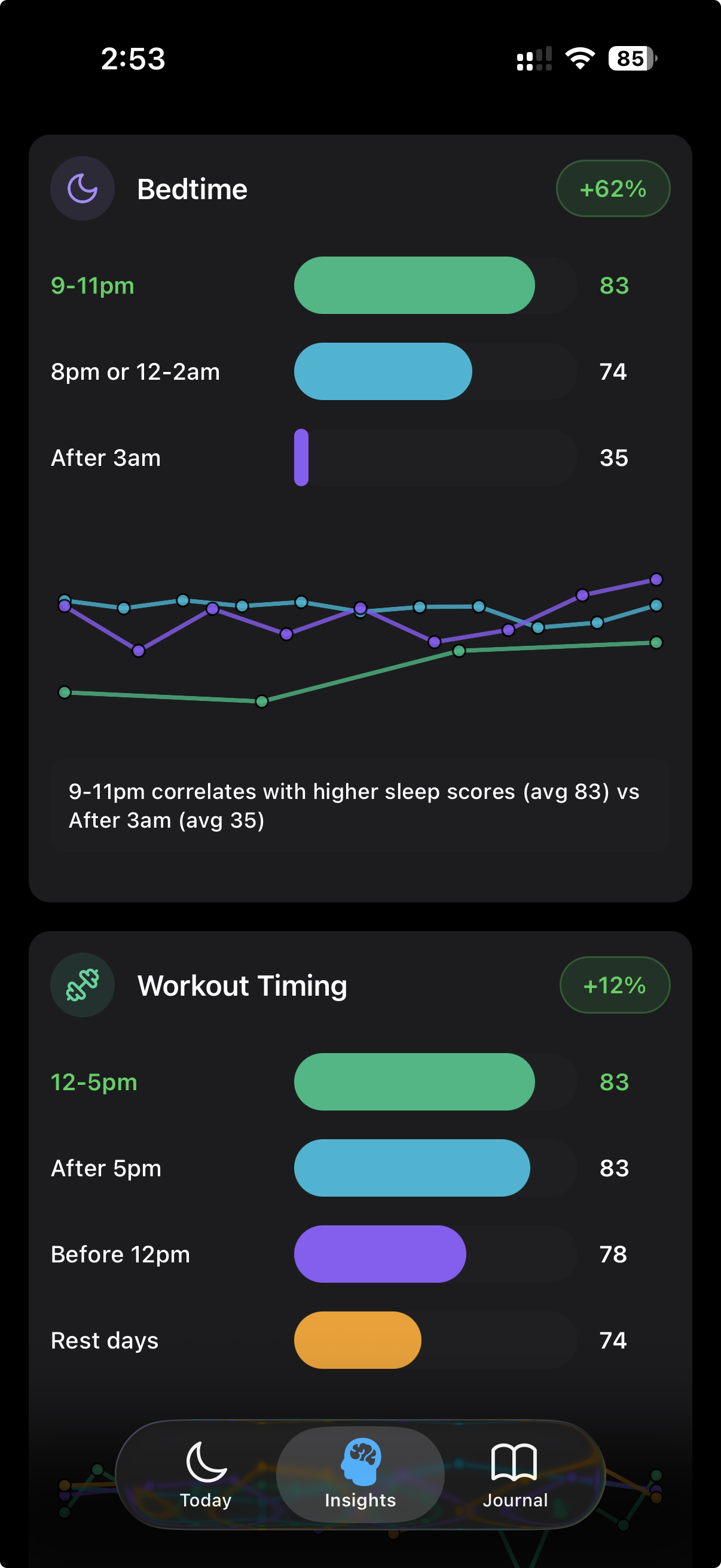
Sleep Efficiency Explained
The other key sleep metric — how much of your time in bed is actually sleep.
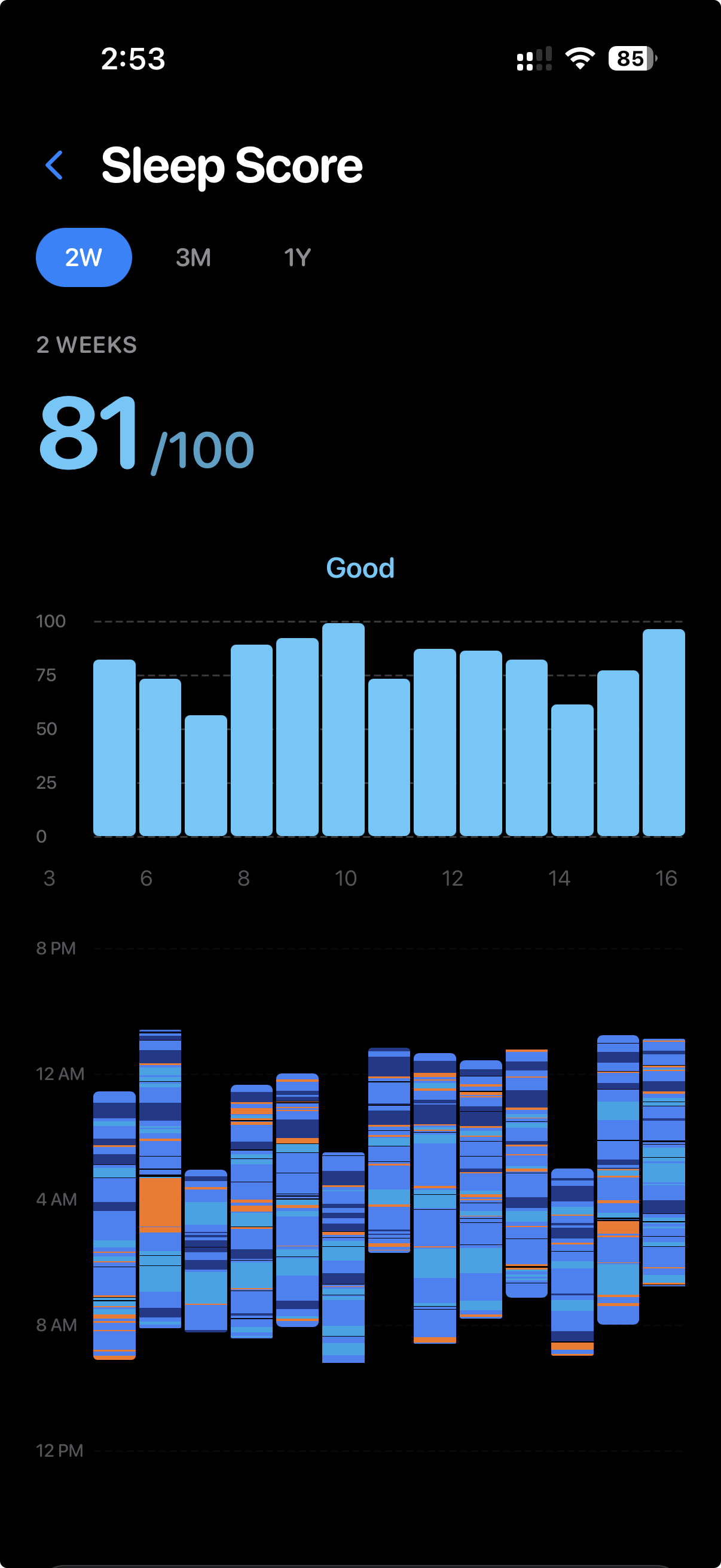
How to Fall Asleep Faster
Nine science-backed tactics to bring your sleep latency into the healthy range.
Track Your Sleep Latency with Reverie
See whether your sleep onset is in the healthy range — or signaling something to fix. Reverie turns your Apple Watch data into a clear picture of how you're sleeping.
Free beta access. Shape the product. First to get updates. Requires Apple Watch.
Written by the Reverie Team
Based on sleep research and scientific studies