Snoring: Causes, Fixes, and When It Becomes Sleep Apnea
Snoring sounds harmless. Sometimes it is. Sometimes it's the loudest warning sign your body has that you've stopped breathing in your sleep. Telling those two cases apart is what this guide is about.
Key Insight: Snoring is air fighting through a narrowed airway. Sometimes it's just noise. When it comes with gasps, pauses, or daytime exhaustion, it's likely obstructive sleep apnea — and that's a different problem with different fixes.
What Actually Makes the Sound
When you fall asleep, the muscles in your throat relax. The soft palate, the tongue, and the tissue at the back of your throat all loosen. Air passing in and out has less room to move, and the soft tissue starts to vibrate. That vibration is the snore.
Three main spots produce the sound. The soft palate (the floppy part at the back of the roof of your mouth) is the most common. The base of the tongue is the second. Nasal turbulence — air whistling past a deviated septum or congested sinus — is the third.
Snoring is extremely common. Population studies put habitual snoring at roughly 30 to 50 percent of adult men and 20 to 40 percent of adult women, with the numbers rising with age. Most of that snoring is "primary" — annoying but medically harmless. A subset of snorers have something more serious.
Three Sound Sources
Who Snores and Why
Snoring isn't random. The same handful of factors show up in study after study. Some you can change, some you can't.
Body Weight
Extra tissue around the neck and tongue narrows the airway. Even modest weight gain can convert silent sleepers into loud snorers. Our piece on sleep and weight loss explains the two-way relationship — bad sleep makes weight gain easier, and that weight then makes the snoring worse.
Sleeping on Your Back
Gravity pulls your tongue and soft palate toward the back of your throat. Many people only snore in the supine position. Researchers call this "positional" snoring, and it's one of the easiest things to fix.
Alcohol Before Bed
Alcohol is a muscle relaxant. It loosens the same throat tissue that causes snoring, which is why a quiet sleeper after a normal night becomes a chainsaw after wine. The full breakdown is in our alcohol and sleep article.
Anatomy You Were Born With
A long soft palate, a thick neck, a small jaw set back, large tonsils, or a deviated septum all narrow the airway. You can't change your anatomy — but you can work around it with positioning and devices.
Age
Throat muscles lose tone with age. Snoring rates climb steadily through the 40s and 50s, and many lifelong silent sleepers start snoring around menopause as muscle tone shifts.
Nasal Congestion
Allergies, colds, and dry air all make you breathe through your mouth. Mouth breathing pulls the jaw back and amplifies the soft palate flutter. Many "snorers" are really just stuffy noses in disguise.
Snoring vs. Sleep Apnea
Here's the line that matters. Primary snoring is loud breathing. Obstructive sleep apnea (OSA) is repeated airway collapse — your throat fully closes, your breathing stops for ten or more seconds, and your brain has to jolt you to a lighter stage of sleep to restart it.
That cycle can repeat dozens of times an hour. Sleep doctors measure it with the Apnea-Hypopnea Index (AHI), which counts breathing events per hour. Five to fifteen is mild apnea. Fifteen to thirty is moderate. Above thirty is severe. Untreated apnea is a serious risk factor for high blood pressure, heart disease, stroke, and diabetes.
You can't always tell from inside your own head. Most people with apnea don't remember waking. Bed partners are usually the first to notice the pauses and the gasping. If you sleep alone, an Apple Watch can sometimes flag the pattern. We cover that in our piece on sleep apnea and Apple Watch.
Warning Signs Snoring Has Crossed Into Apnea
- • Witnessed breathing pauses during sleep
- • Loud gasping, choking, or snorting that wakes you up
- • Morning headaches
- • Daytime sleepiness even after a full 8 hours
- • Dry mouth or sore throat on waking
- • High blood pressure that won't respond to medication
- • Frequent nighttime urination
If three or more of those sound familiar, ask your doctor about a sleep study. It can be done at home now — a small device clipped to your finger and chest, one night, mailed back. The diagnosis is straightforward and the treatments are very good.
What Actually Works to Stop Snoring
These are the fixes with real evidence behind them. Stack the ones that fit your situation.
Sleep on Your Side
Positional therapy is the highest-leverage change for most snorers. Studies of positional OSA patients show measurable drops in snoring loudness and AHI when people stay off their backs. The classic trick is the tennis ball in the back of a t-shirt. Modern positional devices use a small vibrating sensor that nudges you onto your side.
Lose Weight If You're Overweight
Weight loss has a dose-response relationship with apnea severity — the more you lose, the more apnea improves. The MIMOSA randomized trial in JCSM showed Mediterranean diet plus lifestyle change produced meaningful AHI reductions on top of CPAP. Even 5 to 10 percent body weight loss can quiet snoring substantially.
Cut Alcohol in the Evening
Don't drink within three hours of bed. The relaxation effect on throat muscles is dose-dependent — even one drink can convert a quiet night into a noisy one. This is one of the easiest changes and one of the most reliable.
Oral Appliances
Mandibular advancement devices (MADs) hold your lower jaw slightly forward, opening the airway. Meta-analyses show meaningful AHI reductions and better sleepiness scores. They're the first-line treatment for mild-to-moderate OSA in patients who can't tolerate CPAP, and they help most simple snorers too. A dentist trained in dental sleep medicine fits one custom.
CPAP for Diagnosed Apnea
Continuous Positive Airway Pressure pushes a steady stream of air through your airway to keep it from collapsing. Modern machines are quiet, the masks are smaller, and the data improvement on the first night is often dramatic. CPAP is for diagnosed apnea, not for primary snoring — but if you have apnea, nothing else comes close.
Treat Nasal Congestion
Nasal strips, saline rinses, treating allergies, or fixing a deviated septum can all reduce nasal-turbulence snoring. They won't fix apnea, but if your snoring is whistly and high-pitched, this is the place to start.
What Doesn't Really Work
Walk into a pharmacy and you'll see shelves of anti-snoring products. Most have weak or no evidence behind them.
OTC Throat Sprays
Most snore sprays are saline or oil mixtures. Trials show small short-term effects at best. They don't address the underlying airway collapse.
Mouth Taping
Mouth taping has gone viral but the evidence is thin. It may help mild mouth-breathing snorers, but it can be unsafe if you have undiagnosed apnea — you may need to mouth-breathe to recover from an event. Talk to a doctor first.
Anti-Snore Pillows
Most don't do anything. The exceptions are pillows specifically designed to keep you on your side — those work because they're a form of positional therapy.
Sleeping Pills
Sedatives relax airway muscles further. They make snoring and apnea worse, not better. If you're on one, ask your doctor whether it could be aggravating your nighttime breathing.
When to See a Sleep Doctor
See a doctor if your partner reports breathing pauses, if you wake up gasping, if you're exhausted during the day despite a full night in bed, or if you have high blood pressure that resists treatment. These are not "wait and see" symptoms.
A home sleep study is usually the first step. It's covered by most insurance, it takes one night, and the results give you a clear AHI number. From there your doctor can recommend CPAP, an oral appliance, surgery in some cases, or just confirm that your snoring is primary and the simple fixes are enough.
How Reverie Helps You Track the Pattern
Reverie shows you which nights have fragmented sleep — the kind of pattern apnea produces. You can tag drinks, sleep position, and weight changes to see what moves the needle.
- • Spot fragmented nights that may need a sleep study
- • Tag positional habits and see the difference
- • Track snoring fixes over weeks, not nights
- • Get a sleep score that reflects continuous, restorative sleep
References
- Young T, et al. "Prevalence and correlates of snoring and observed apneas in 5,201 older adults." Sleep. 1996;19(7):531-538. PubMed
- de Ruiter MHT, et al. "Treatment of snoring with positional therapy in patients with positional obstructive sleep apnea syndrome." Scientific Reports. 2015;5:18188. Nature
- Georgoulis M, et al. "Dose-response relationship between weight loss and improvements in obstructive sleep apnea severity (MIMOSA trial)." Journal of Clinical Sleep Medicine. 2022. JCSM
- Ramar K, et al. "Clinical Practice Guideline for the Treatment of Obstructive Sleep Apnea and Snoring with Oral Appliance Therapy." JCSM. 2015;11(7):773-827. PubMed Central
- Manetta IP, et al. "Long-term efficacy of mandibular advancement devices in adult OSA: A systematic review and meta-analysis." 2023. PubMed Central
- Ebrahim IO, et al. "Alcohol and sleep I: effects on normal sleep." Alcohol Clin Exp Res. 2013;37(4):539-549. PubMed
Related Articles
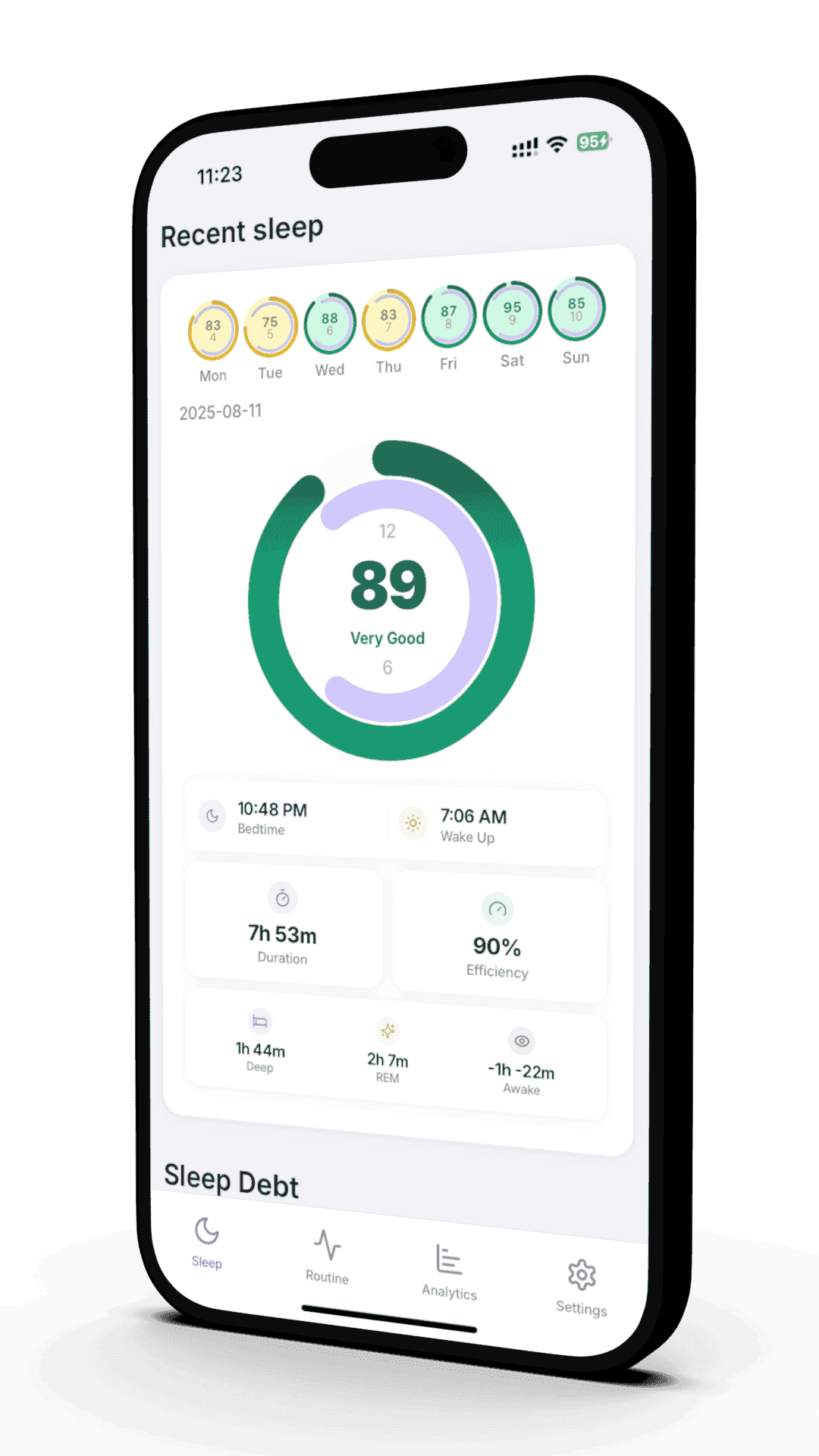
Sleep Apnea Detection with Apple Watch
How Apple Watch flags possible apnea and what to do if it does.
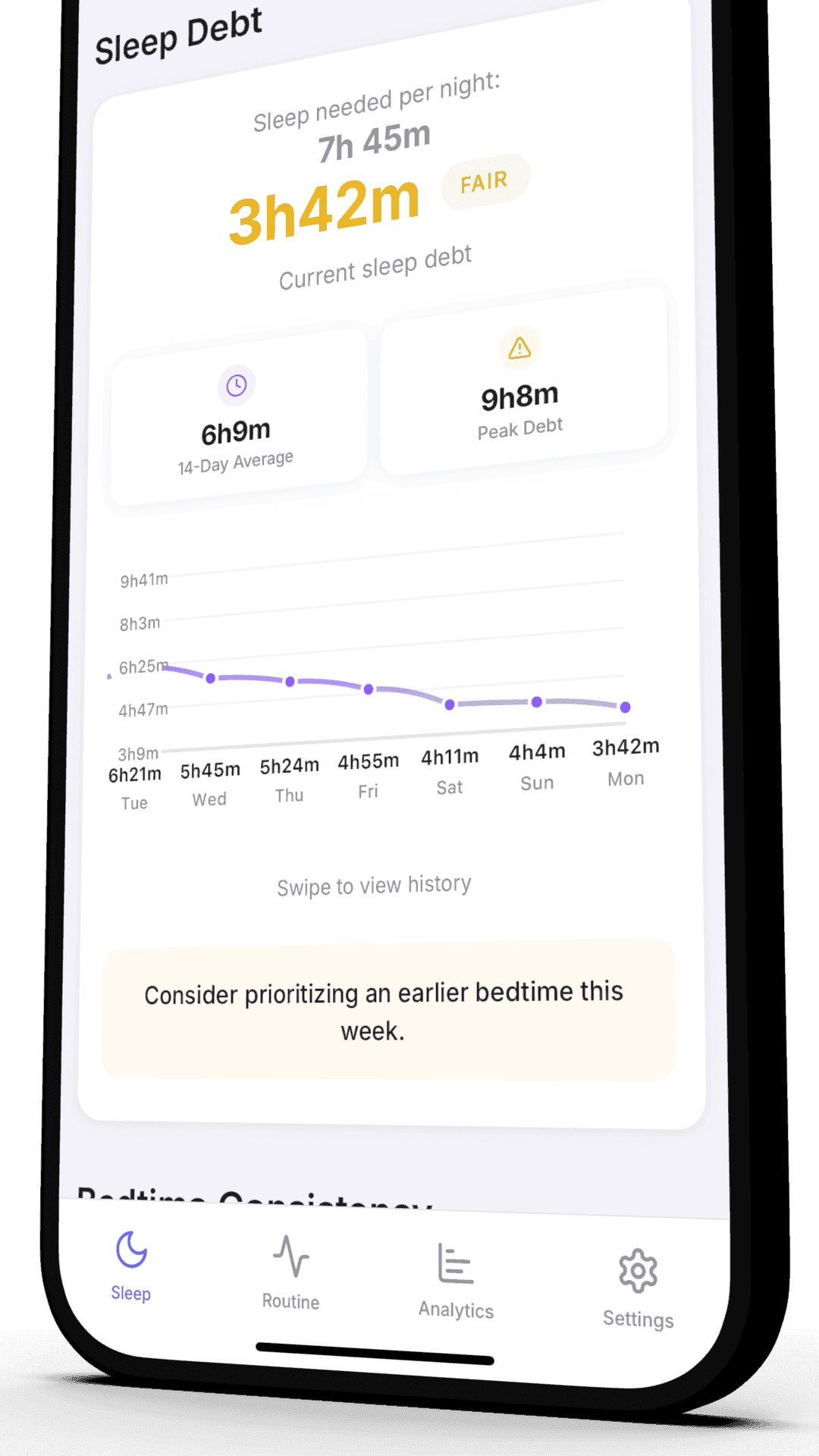
Sleep and Weight Loss
The two-way link between snoring, sleep, and body weight.
Track What's Disrupting Your Sleep
Reverie turns Apple Watch sleep data into clear nightly reports. Spot fragmented nights, tag the habits behind them, and watch your sleep score respond.
Free beta access. Shape the product. First to get updates. Requires Apple Watch.
Written by the Reverie Team
Based on sleep research and scientific studies